Sparky: As promised some boring stuff to make a point ... as when some don't get they are a menace to public health ...
Typhoid Mary AKA Mary Mallon

Typhoid Mary in a 1909 newspaper illustration
Mary Mallon (September 23, 1869 – November 11, 1938), also known as Typhoid Mary, was an Irish immigrant who was the first known healthy carrier of typhoid in the United States. She contracted a mild case of typhoid fever but was never cured, so she spread the disease to others. Having no particular job skills she obtained employment in private homes around New York City, eventually obtaining the relatively well-paid position of household cook.
Birth and emigration
She was born in Cookstown, County Tyrone, Ireland in 1869 and emigrated to the United States by herself in 1883.Cook
Mary worked as a cook in the New York City area between 1900 and 1907. During this part of her working career she infected 22 people with the disease, one of whom died. Mary was a cook in a house in Mamaroneck, New York, for less than two weeks in the year 1900 when the residents came down with typhoid. She moved to Manhattan in 1901, and members of that family developed fevers and diarrhoea, and the laundress died. She then went to work for a lawyer, until seven of the eight household members developed typhoid. Mary spent months helping to care for the people she made sick, but her care further spread the disease through the household. In 1904, she took a position on Long Island. Within two weeks, four of ten family members were hospitalized with typhoid. She changed employment again, and three more households were infected. Frequently, the disease was transmitted by a dessert of iced peaches, her favorite recipe.
Typhoid
George Soper, a sanitary engineer hired by the landlord of a house where Mary had worked for typhoid fever victims, after careful investigation identified Mary as the carrier. He approached her with the news that she was spreading typhoid. She violently rejected his request for urine and stool samples, and Soper left, later publishing his findings in the June 15, 1907 issue of the Journal of the American Medical Association. Soper brought a doctor with him on his next contact with Mallon, but was again turned away.
Mallon's denials that she was a carrier were based in part on the diagnosis of a reputable chemist; he found she was not harboring the germs. While she was merely in temporary remission, the diagnosis contributed to Mallon's refusal to accept the allegations. Moreover, when Soper first told her she was a carrier, the concept that a person could spread disease and remain healthy was not well known. Finally, George Soper was generally tactless in his dealings with her. (During one encounter, he told her he would write a book about her -- and give her all the royalties. She got up, walked to the bathroom, and locked the door. Soper got up and left.)
Quarantine
The New York City Health Department sent Dr. Josephine Baker to talk to Mallon, but "by that time she was convinced that the law was wantonly persecuting her, when she had done nothing wrong." [1]
Mary Mallon in a hospital bed. She was forcibly quarantined as a carrier of typhoid fever in 1907 for three years and then again from 1915 until her death in 1938.
A few days later Baker arrived at her place of work with several police officers to take her into custody. Baker had to sit on Mary to keep her from leaving. The New York City health inspector investigated and found her to be a carrier, isolating her for three years at a hospital located on North Brother Island, and then releasing her on the condition she did not work with food. However in 1915 she returned to cooking and infected 25 people while working as a cook at New York's Sloan Hospital; two of those she infected died. Public health authorities then again seized her and confined Mary Mallon in quarantine for life. She became something of a celebrity, and was interviewed by journalists, who were forbidden to accept as much as a glass of water from her. Later in life, she was allowed to work in the island's laboratory as a technician.
Death
Mary's eventual death (in 1938) was due to pneumonia, not typhoid. However, an autopsy found evidence of live typhoid bacteria in her gallbladder. Her body was incinerated in Saint Raymond's Cemetery in the Bronx.
Legacy
Part of the problems Mary had resulted from her vehement denial of the situation. She maintained she was healthy and had never had typhoid fever. Historians say it also stemmed from the prejudice that existed against working-class Irish immigrants at the time. Today, a Typhoid Mary is a term for a carrier of a dangerous disease who is a danger to the public because they refuse to take appropriate precautions or cooperate with the authorities to minimize the risk.
Popular Culture
- In Chris Elliot's book, The Shroud of the Thwacker, Elliot is sent back in time, suspected to be the Thwacker (serial killer). He is given cover by Mary Mallon because she is attracted to him. When the police come to arrest her (Elliot believes it is himself the police are coming for) she "forcefully pulled me (Elliot) to her and planted a wet slobbering kiss on my lips. I tried to pull away but she was too strong for me...She took a breath and coughed in my face and then dove into my mouth again..." Elliot later remembers the importance of Mary Mallon and feels symptoms of typhoid coming on. He quickly kills the infection with some amoxicillin he left in his coat pocket while traveling back in time.
- Typhoid Mary is the name of a Marvel comic book villain, though her powers and origin have nothing to do with the historical figure.
- Mark St. Germain wrote a play about Mallon called A Plague of Angels.
Further reading
- Typhoid Mary, Captive to the Public's Health, Judith Walzer Leavitt, Beacon Press, Boston, 1996, hardcover, 331 pages, ISBN 0-8070-2102-4
- Quarantine: The Story of Typhoid Mary, Mercedes Graf, Vantage Press, New York, 1998, paperback, 133 pages, ISBN 0-5331-2512X
- Fighting for Life, Sara Josephine Baker, Macmillan Press, New York 1939
- The Ballad of Typhoid Mary, J.F. Federspiel [translated by Joel Agee], Ballantine Press, New York, 1985
External links
- "Dinner with Typhoid Mary," Long Island History
- A more detailed profile of Typhoid Mary
- PBS NOVA site: "The Most Dangerous Woman in America"
Shingles or Herpes zoster
| ICD-10 | B02 |
|---|---|
| ICD-9 | 053 |
| DiseasesDB | 29119 |
| MedlinePlus | 000858 |
| eMedicine | med/1007 |
Herpes zoster, colloquially known as shingles, is the reactivation of varicella zoster virus, leading to a crop of painful blisters over the area of a dermatome. In Italy and in Malta, it is sometimes referred to as St. Anthony's fire. It occurs very rarely in children and adults, but its incidence is high in the elderly (over 60), as well as in any age group of immunocompromised patients. It affects some 500,000 people per year in the United States. Treatment is generally with antiviral drugs such as aciclovir. Many patients develop a painful condition called postherpetic neuralgia which is often difficult to manage.
In some patients, herpes zoster can reactivate subclinically with pain in a dermatomal distribution without rash. This condition is known as zoster sine herpete and may be more complicated, affecting multiple levels of the nervous system and causing multiple cranial neuropathies, polyneuritis, myelitis, or aseptic meningitis.
The word herpes comes from the Greek word for snake; it is cognate with herpetology[1].
Signs and symptoms
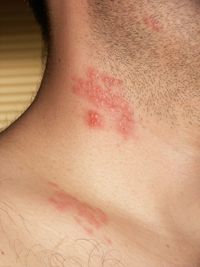
Often, pain is the first symptom. This pain can be characterized as stinging, tingling, numbing, or throbbing, and can be pronounced with quick stabs of intensity. Then 2-3 crops of red lesions develop, which gradually turn into small blisters filled with serous fluid. A general feeling of unwellness often occurs. In some cases, the rash does not form blisters, but has an appearance much like urticaria ("hives").
As long as the blisters have not dried out, HZ patients may transmit the virus to others. This could lead to chickenpox in people (mainly young children) who are not yet immune to this virus.
Shingles blisters are unusual in that they only appear on one side of the body. That is because the chickenpox virus can remain dormant for decades, and does so inside the spinal column or a nerve fiber. If it reactivates as shingles, it affects only a single nerve fiber, or ganglion, which can radiate to only one side of the body. The blisters therefore only affect one area of the body and do not cross the midline. They are most common on the torso, but can also appear on the face (where they are potentially hazardous to vision) or other parts of the body.
Diagnosis
The diagnosis is visual — very few other diseases mimic herpes zoster. In case of doubt, fluid from a blister may be analysed in a medical laboratory.
Pathophysiology
The causative agent for herpes zoster is varicella zoster virus (VZV). Most people are infected with this virus as a child, as it causes chickenpox. The body eliminates the virus from the system, but it remains dormant in the ganglia adjacent to the spinal cord (called the dorsal root ganglion) or the ganglion semilunare (ganglion Gasseri) in the cranial base.
Generally, the immune system suppresses reactivation of the virus. In the elderly, whose immune response generally tends to deteriorate, as well as in those patients whose immune system is being suppressed, this process fails. (Some researchers speculate that sunburn and other, unrelated stresses that can affect the immune system may also lead to viral reactivation.) The virus starts replicating in the nerve cells, and newly formed viruses are carried down the axons to the area of skin served by that ganglion (a dermatome). Here, the virus causes local inflammation in the skin, with the formation of blisters.
The pain characteristic of herpes zoster is thought to be due to irritation of the sensory nerve fibers in which the virus reproduces.
Therapy
Aciclovir (an antiviral drug) inhibits replication of the viral DNA, and is used both as prophylaxis (e.g., in patients with AIDS) and as therapy for herpes zoster. Other antivirals are valaciclovir and famciclovir. Steroids are often given in severe cases. During the acute phase oral aciclovir should be given five times daily for 7 to 10 days. Immunocompromised patients may respond best to intravenous aciclovir. In patients who are at high risk for recurrences, an oral dose of aciclovir, taken twice daily, is usually effective.
The long term complication postherpetic neuralgia may cause persistent pain that lasts for years. Pain management is difficult as conventional analgesics may be ineffective. Alternative agents are often used, including tricyclic antidepressants (particularly amitriptyline), anticonvulsants (e.g. gabapentin, and/or topical capscaicin).
A vaccine called live attenuated Oka/Merck VZV that has been developed by Merck & Co. has proven successful in preventing half the cases of herpes zoster in a study of 38,000 people who received the vaccine. The vaccine also reduced by two-thirds the number of cases of postherpetic neuralgia (Oxman et al., 2005). However, prior to the vaccine, it has long been known that adults received natural immune boosting from contact with children infected with varicella. This helped to suppress the reactivation of herpes zoster. In Massachusetts, herpes zoster incidence increased 90%, from 2.77/1000 to 5.25/1000 in the period of increasing varicella vaccination 1999-2003 (Yih et al., 2005). The effectiveness of the varicella vaccine itself is dependent on this exogenous (outside) boosting mechanism. Thus, as natural cases of varicella decline, so has the effectiveness of the vaccine (Goldman, 2005).
Often the same treatment given to burn victims relieves the pain of shingles, including over-the-counter moist burn pads.
Prognosis
The rash and pain usually subside within 3 to 5 weeks. The most common chronic complication of herpes zoster is postherpetic neuralgia. Pain that persists for longer than one to three months after resolution of the rash is generally accepted as the sign of postherpetic neuralgia. Sometimes serious effects including partial facial paralysis (usually temporary), ear damage, or encephalitis may occur. Shingles on the upper half of the face (the first branch of the trigeminal nerve) may result in eye damage and require urgent ophthalmological assessment. Ocular complications occur in approximately one half of patients with involvement of the ophthalmic division of the trigeminal nerve. These complications include mucopurulent conjunctivitis, episcleritis, keratitis and anterior uveitis. Cranial nerve palsies of the third, fourth and sixth cranial nerves may occur, affecting extraocular motility.
Since shingles is a reactivation of a virus contracted previously—often decades earlier—it cannot be induced by exposure to another person with shingles or chickenpox. Those with active blisters, however, can spread chickenpox to others who have never had that condition and who have not been vaccinated against it.
References
- G.S. Goldman. Medical Veritas Internation Inc. (2005). "Universal varicella vaccination: efficacy trends and effect on herpes zoster". International Journal of Toxicology 24 (4): 205-213. PMID 16126614.
- M.N. Oxman et al. The Shingles Prevention Study Group (2005). "A vaccine to prevent herpes zoster and postherpetic neuralgia in older adults". New England Journal of Medicine 253 (22): 2271-2284. PMID 15930418.
- W.K. Yih et al. Department of Ambulatory Care and Prevention, Harvard Medical School and Harvard Pilgrim Health Care (2005). "The incidence of varicella and herpes zoster in Massachusetts as measured by the Behavioral Risk Factor Surveillance System (BRFSS) during a period of increasing varicella vaccination coverage, 1998-2003". BMC Public Health 5 (1): 68-68. PMID 15960856.
Notes and references
- ^ Treatment of Herpes Zoster with Fire Needle retrieved May 22, 2006
External links
- NIH Facts About Shingles
- NINDS shingles
- eMedicine:Consumer 17511-1
- Center for Disease Control National Immunization Program Information on Shingles
- Herpes Online Information on Shingles
- National Health Service 335
- United States Food and Drug Administration (FDA) information page (This article originally appeared in the May-June 2001 FDA Consumer and contains revisions made in June 2005)
- Information about management of Shingles for physicians
- Shingles page on GANFYD.org medical wiki
- Links to pictures of Shingles (Hardin MD/Univ of Iowa)